A Case Report: Pseudohypoparathyroidism (PHP)
Oputa RN1*, Onumonu EN2, Oputa PU3and Chinenye S4
1Department of Internal Medicine, Federal Teaching Hospital Owerri. Owerri. Imo State
2Department of Radiology, Federal Teaching Hospital Owerri. Owerri. Imo State
3Lagos State Government, National Youth Service Corp (NYSC). Nigeria
4Department of Internal Medicine, University of Port Harcourt Teaching Hospital (UPTH). Port Harcourt. Rivers State. Nigeria
*Corresponding author
Oputa RN, 1Department of Internal Medicine, Federal Teaching Hospital Owerri. Owerri. Imo State
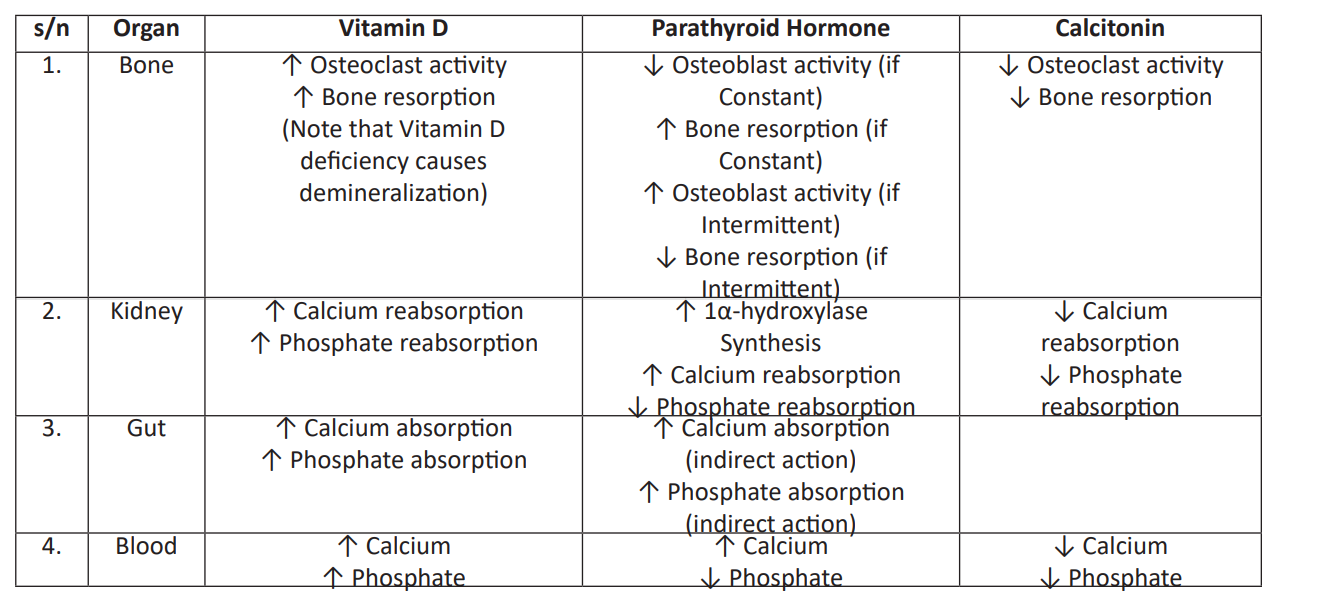
Table 1: Comparative actions of Vitamin D, Parathyroid Hormone (PTH), and Calcitonin.
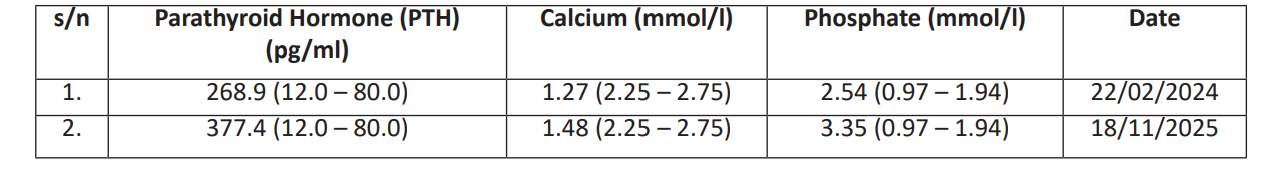
Table 2:Laboratory Results with dates.
3. Magnesium = 0.63 mmol/l (0.65 – 0.95) – (22/02/2024)
4. Vitamin D (25 OH) = 19.2 ng/ml (> 20.0) – (18/11/2025)
5. ESR = 35 mm/hr. (0 – 20)
6. Blood Group = A Rh D +
7. Haemoglobin = 11.5 g/dl (13 – 18)
8. SE/U/Cr: Normal: Na 146.3 (135-150), K 4.1 (3.5-5.0), Cl 98 (96-
108), Urea 20 (15-40), Creatinine 1.1 (0.5-1.5).
9. Urinalysis = Normal.
10. CT scan of the neck (21/11/2025): unremarkable.
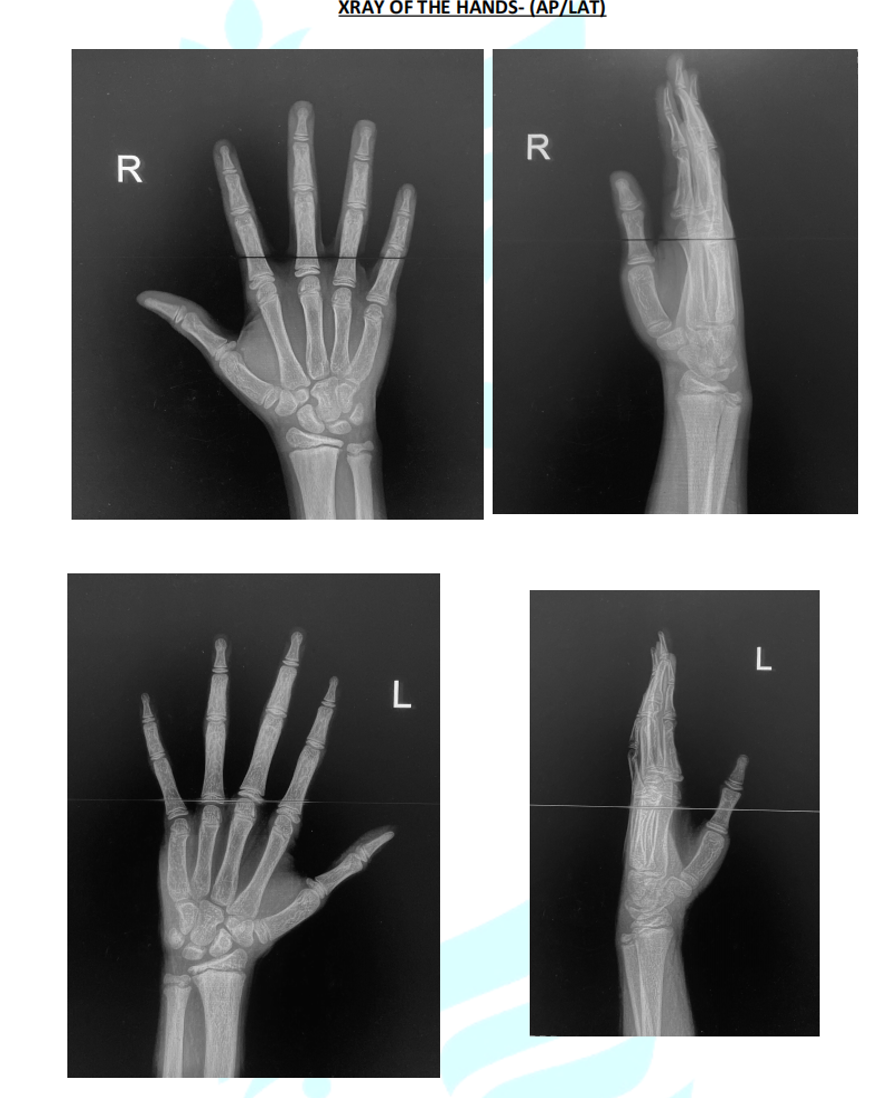
11. X-Ray of both hands: see Figure 1.
Figure 1: X-Ray of the Hands- (AP/LAT).
- Scanlon VC, Sanders T Parathyroid Gland. Essentials of Anatomy and Physiology.Chapter 10. (7th edn), pp. 264.
- Holt RIG, Hanley NA. Calcium and Metabolic Bone Disorder. Essential Endocrinology and Diabetes. Chapter 9, (6th edn), pp. 190 - 212.
- Shoback DM, Schafer AL, Bikle DD. Metabolic Bone Disese. Greenspan’s Basic and Clinical Endocrinology. Chapter 8, (10th edn), pp. 239 - 297.
- Bilezikian JP, Walker MD, Binkley N, Goltzman D, Mannstadt M. Hormones and Disorders of Mineral Metabolism. Williams Textbook of Endocrinology. Chapter 27, (15th edn), pp. 1171 - 1226.
- Abbas A. Diagnosis and management of hypocalcaemia in adult (Case 16). Endocrinology and Diabetes: Cases Studies, Questions and Commentaries. Case 16, (1st edn), pp. 133 - 140. Editors (Springer): Ramzi Ajjan and Stephen M Orme.