Orofacial injuries (OFIs) are a major subset of trauma-related conditions and represent a serious global public health issue. These injuries affect the face, mouth, jaws, and associated soft tissues, often leading to significant functional, psychological, and aesthetic complications. According to Yi [1], the global incidence of facial fractures was approximately 10.7 million cases in 2019, accounting for nearly one-seventh of all bone fractures worldwide. Despite their burden, orofacial injuries remain underrepresented in trauma research and public health interventions, particularly in low- and middle-income countries (LMICs).
Orofacial injuries have diverse etiologies, including road traffic accidents (RTAs), interpersonal violence, falls, and sports-related incidents [2]. Children are especially vulnerable due to their developing motor coordination. In early childhood, most injuries affect the primary dentition between ages two and three, primarily from domestic falls [3]. Unfortunately, trauma to primary teeth is often neglected under the assumption that the teeth will naturally exfoliate, resulting in long-term developmental and psychological effects.
In sub-Saharan Africa, RTAs, assaults, and falls remain the dominant causes of orofacial trauma [4]. The high rates of motorization, poor enforcement of road safety laws, and increasing interpersonal violence contribute significantly to this pattern. OFIs frequently cause speech impairment, difficulty in eating and breathing, and social withdrawal due to facial disfigurement. Their management often requires multidisciplinary intervention-spanning oral and maxillofacial surgery, emergency medicine, and psychological support which imposes substantial economic and healthcare burdens.
In Zambia, and particularly in Lusaka, rapid urbanization, increased motor vehicle usage, and widening socioeconomic inequalities have heightened the risk of trauma. Despite these developments, empirical data on orofacial injuries remain sparse. Most trauma studies conducted in Zambia aggregate data across all injury types, obscuring the epidemiological profile and specific determinants of OFIs. Levy Mwanawasa University Teaching Hospital (LMUTH), a tertiary-level referral institution, presents an ideal setting to conduct a detailed investigation into these injuries. A case-control study comparing patients with and without orofacial injuries would allow for the identification of risk factors, quantification of their effects, and generation of local evidence for policy and clinical practice.
Although trauma-related injuries are common in Lusaka, there is a marked absence of hospital-based research specifically examining orofacial injuries. Existing studies fail to disaggregate trauma data by anatomical region, limiting understanding of OFIs’ distinct epidemiological characteristics. Consequently, high-risk populations, behavioural correlates, and environmental determinants remain poorly identified. This data gap hampers the formulation of targeted interventions for prevention and management.
2.1 Risk Factors and Epidemiological Trends in Orofacial Injuries
Orofacial injuries (OFIs) represent a significant global public health concern, with substantial variation in epidemiological patterns across regions. According to recent findings from the Global Burden of Disease Study, incident cases and the associated disability burden of OFIs have increased globally over the past three decades [1]. Males, particularly young adults, remain the most affected demographic, and falls and road injuries are consistently identified as the primary causes of facial fractures. The burden tends to increase with age, especially in terms of years lived with disability (YLDs), underscoring the long-term consequences of these injuries.
In sub-Saharan Africa, orofacial trauma is frequently linked to road traffic accidents (RTAs), interpersonal violence, and falls. For example, a Nigerian hospital-based study identified RTAs as the leading cause of maxillofacial injuries, accounting for 48.2% of cases, followed by assaults (25.6%) and falls (18.3%) (Ndung’u, 2017). In Tanzania, OFIs constituted a large proportion of trauma admissions, predominantly affecting males aged 20–30 years [5]. A similar pattern was observed in Ethiopia, where RTAs emerged as the primary cause of facial fractures among trauma patients [6].
Dental trauma, a critical subset of OFIs, shows distinct patterns in terms of risk exposure. A systematic review by Esses [7] highlighted traumatic dental injuries as a major issue globally, particularly among children aged 2–3 years. At this developmental stage, children are more prone to falls due to immature motor coordination. Physical abuse is also a significant contributor to pediatric OFIs. South African hospital data revealed that in 59% of confirmed child abuse cases, orofacial trauma was present most commonly involving injuries to the lips [8,9].
In Zambia, specific data on OFIs remain scarce. However, the limited existing research points to increasing rates of orofacial trauma, largely due to rapid urbanization, growing vehicle use, and socioeconomic disparities. At the University Teaching Hospital (UTH) in Lusaka, one study reported that RTAs accounted for 42.3% of maxillofacial injuries [10]. Another investigation found that males represented the majority of OFI cases, supporting the trend seen elsewhere in sub-Saharan Africa [11]. These patterns emphasize the importance of conducting case-control studies to better understand and quantify the specific risk factors for OFIs in local settings like Zambia, where systemic challenges such as weak traffic law enforcement and limited access to surgical care may exacerbate injury outcomes [12].
Understanding these risk factors is essential for developing context-specific prevention strategies and health system responses. By identifying individual and environmental contributors to orofacial trauma, targeted interventions can be more effectively designed, particularly in high-risk populations.
2.2 Socio-Demographic Characteristics of OFI Patients
Demographic factors significantly influence OFI susceptibility, with consistent patterns observed across multiple studies. A systematic review by [13] established that males aged 15–30 years face the highest OFI risks globally, primarily due to risk-taking behaviours and occupational exposures. Kenyan data revealed that 72% of maxillofacial trauma patients were males aged 18–35 years, with RTAs and violence being predominant causes14. Similar trends were documented in Ethiopia, where 78.6% of facial fracture patients were males, peaking in the 20–29 age group [14,15].
Pediatric populations represent another vulnerable demographic. A Brazilian study found that children under 6 years accounted for 31.2% of dental trauma cases, with falls being the leading mechanism [16]. South African research highlighted that toddler (2–3 years) had the highest primary tooth trauma rates due to motor skill development [1], School-aged children also face significant risks, with sports-related dental injuries affecting 18.6% of adolescents in U.S. studies [17].
Socioeconomic status and occupation further modulate OFI risks. In Ghana, commercial motor riders constituted 38.7% of OFI cases, correlating with poor helmet compliance [18]. Zambian studies identified informal sector workers as particularly vulnerable due to limited occupational safety measures [11], Urban-rural disparities also exist, with urban populations experiencing higher assault-related OFIs, while rural areas report more agricultural and fall-related injuries [12]
2.3 Risk Factors for Orofacial Injuries
Multiple interrelated factors contribute to OFI occurrence, with regional variations in their relative importance. Road traffic accidents emerge as a leading cause globally, particularly in LMICs with weak traffic law enforcement. An Indian study found that 56.3% of facial fractures resulted from motorcycle accidents, with only 12.3% of riders wearing helmets [17], Nigerian data similarly implicated motorcycles in 52.1% of maxillofacial trauma case [17,18].
Alcohol consumption significantly exacerbates OFI risks. South African studies reported alcohol involvement in 42.8% of assault-related facial injuries, Zambian data revealed that 36.4% of assault cases leading to OFIs involved alcohol intoxication [11].
Sports and recreational activities constitute another major risk domain. A systematic review by Glendor19 estimated that sports account for 13–39% of dental trauma cases in adolescents. High-risk activities include basketball (24.1%), soccer (18.9%), and cycling (15.3%) [19]. Protective equipment use remains low in many settings, with mouthguard utilization below 10% in some athlete populations [20].
Environmental and structural factors also play crucial roles. Inadequate playground safety measures contribute to 28.3% of pediatric dental injuries in Brazil (Andrade et al., 2016), Workplace hazards, particularly in construction and mining, account for 15–20% of occupational OFIs in developing nations [21].
An analytical case-control design was employed to identify and quantify risk factors associated with orofacial injuries among patients at LMUTH. The design compared patients with orofacial injuries (cases) to those without (controls), allowing the investigation of multiple exposures simultaneously. This approach was efficient for identifying associations where experimental manipulation was not possible.
Methodology: Research Design
An analytical case-control design was employed to identify and quantify risk factors associated with orofacial injuries among patients at LMUTH. The design compared patients with orofacial injuries (cases) to those without (controls), allowing the investigation of multiple exposures simultaneously. This approach was efficient for identifying associations where experimental manipulation was not possible.
Research Site
The study was conducted at Levy Mwanawasa University Teaching Hospital (LMUTH), located in Lusaka, Zambia. LMUTH is a tertiary referral and teaching hospital providing specialized medical, dental, and surgical care. It serves as a referral center for trauma cases across Lusaka and neighboring provinces, making it ideal for this study. The hospital includes a Maxillofacial Surgery Unit, Accident and Emergency Department, and Dental Clinic, all of which manage orofacial trauma patients.
Study Population
The target population comprised all patients presenting to LMUTH with traumatic injuries (both orofacial and non-orofacial) during the study period. Cases: Patients diagnosed with orofacial injuries (facial fractures, soft-tissue lacerations, dental trauma, or jaw fractures). Controls: Patients without orofacial injuries but presenting with other trauma types (for example, limb fractures, chest trauma) or non-trauma cases attending outpatient departments during the same period. Inclusion and Exclusion Criteria: The study Inclusion Criteria was patients aged five years and above attending LMUTH during the study period. For cases: confirmed diagnosis of orofacial injury. For controls: no evidence of orofacial injury. Those excluded were patients with incomplete medical records and or repeat visits of the same patient.
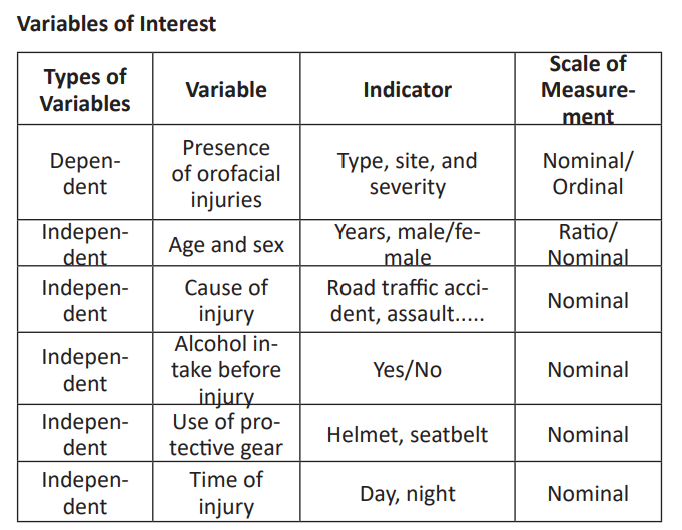
Variables of Interest
Ethical Considerations
Ethical approval was obtained from the Levy Mwanawasa Medical University Biomedical Research Ethics Committee (LMMU-REC 0000917-25) and the LMUTH Ethics Committee. Authority to conduct research was obtained from National Health Research Authority (NHRA) number NHRA9769/03/09/2025 Written informed consent was obtained from all participants. Confidentiality was maintained by omitting names from questionnaires and assigning coded identifiers. Participation was voluntary, and respondents could withdraw at any point without penalty. Data will be stored securely and retained for five years before destruction.
Results
Socio-Demographic Characteristics
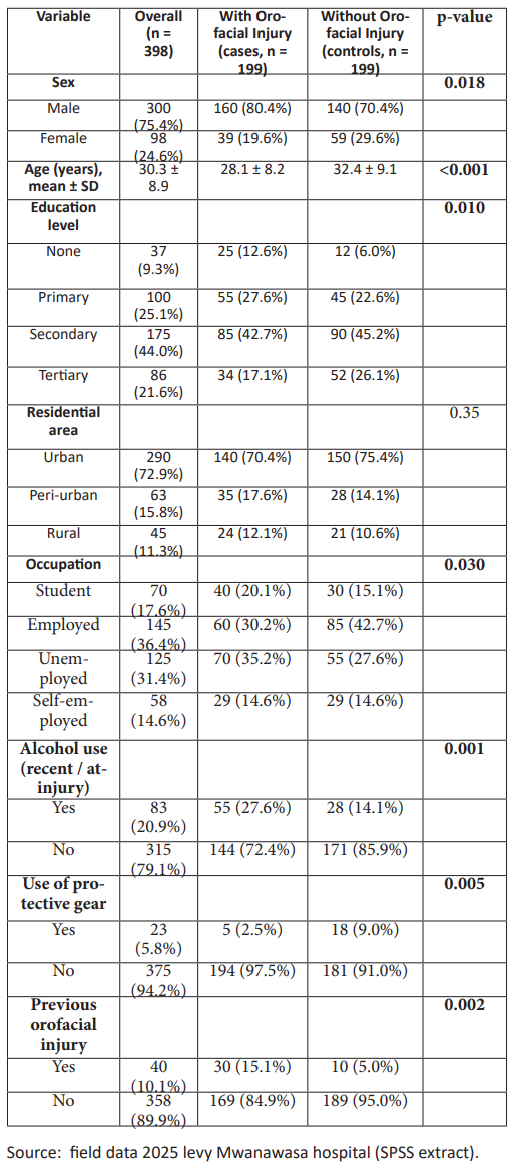
Source: field data 2025 levy Mwanawasa hospital (SPSS extract)
Table 1 presents the socio-demographic distribution of participants with or without orofacial injuries. The findings revealed that a majority of the patients with OFIs were male (80.4%), compared to 70.4% among controls, indicating a statistically significant gender difference (p = 0.018).
The mean age of OFI patients (28.1 ± 8.2 years) was significantly lower than that of controls (32.4 ± 9.1 years), suggesting that younger adults were more prone to facial trauma (p < 0.001). The 21–30-year age bracket was most affected,
In terms of education level, participants with tertiary education were fewer among OFI patients (17.1%) compared to controls (26.1%), and this difference was statistically significant (p = 0.010). The results imply that higher educational attainment may serve as a protective factor against orofacial injuries, possibly through increased awareness and adherence to safety practices. Similarly, occupation showed a significant association with injury status (p = 0.030), with a greater proportion of unemployed or informally employed individuals among the OFI group. Although there was no statistically significant difference in residential area (p = 0.35), most patients were from urban areas, reflecting LMUTH’s location and catchment population. However, this may also highlight urban-related risks such as traffic congestion and interpersonal violence, which contribute to injury prevalence in metropolitan regions.
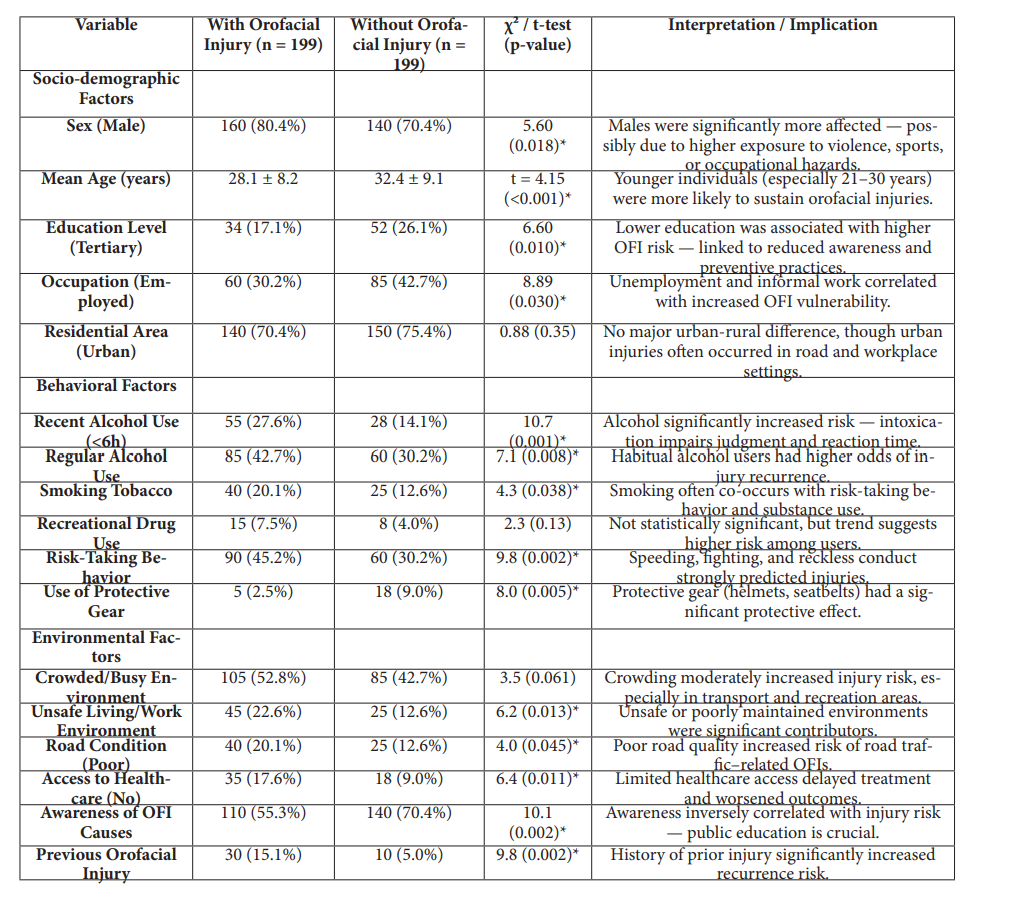
Source: Field Data 2025 Levy Mawanawasa Hospital
Statistically significant at p < 0.05
Table 2 extended the analysis to examine behavioral and environmental factors associated with orofacial injuries. Behavioral factors were found to play a substantial role. Recent alcohol consumption within six hours before injury was strongly associated with OFIs (p = 0.001), while regular alcohol use also showed a significant association (p = 0.008).
Smoking tobacco was also significantly associated with OFIs (p = 0.038). Though not a direct mechanical cause, tobacco use is often linked to risk-taking and violent behaviors. Similarly, risk-taking behavior including fighting, speeding, and failure to use safety gear was significantly associated with OFI occurrence (p = 0.002). Conversely, use of protective gear such as helmets and seatbelts showed a protective effect, with only 2.5% of OFI patients reporting use compared to 9.0% among controls (p = 0.005).
Regarding environmental factors, participants reporting unsafe living or working conditions were significantly more likely to sustain OFIs (p = 0.013). Poor road conditions were another determinant (p = 0.045), indicating that environmental hazards play a contributory role. Limited access to healthcare (p = 0.011) was also a significant predictor, as delayed emergency response and lack of first aid exacerbate injury severity and recovery time. Participants with a previous history of orofacial injury were three times more likely to sustain another (p = 0.002), suggesting that injury recurrence is influenced by unresolved behavioral and environmental factors. Additionally, awareness of OFI causes was inversely correlated with injury occurrence (p = 0.002), demonstrating that preventive education and health promotion are effective deterrents.