Acute lateral patellar dislocation is a common traumatic knee injury in adolescents, and first-time episodes are frequently associated with soft-tissue and osteochondral damage. MRI studies have shown that medial patellofemoral ligament (MPFL) rupture occurs in up to 90% of first-time dislocations [4]. This structural injury contributes significantly to early functional impairment and the risk of recurrent instability. The mechanism typically involves valgus stress combined with external rotation of the tibia. Adolescents are particularly vulnerable because of their higher activity levels and ligamentous laxity. Fithian et al. reported recurrence rates ranging from 15–60% depending on anatomical risk factors [1].
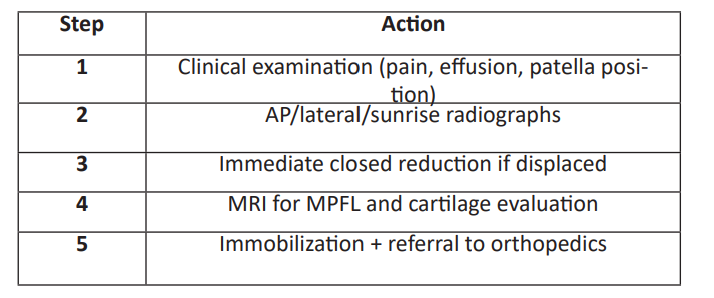
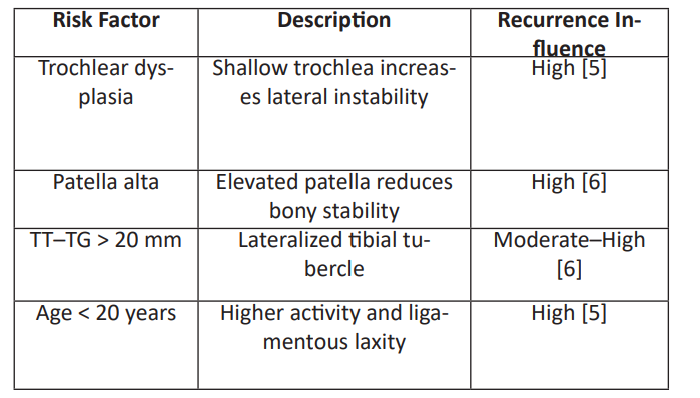
Radiographs are essential initially, while MRI identifies MPFL tears, osteochondral fragments, and risk factors such as trochlear dysplasia or patella alta. Stefancin and Parker emphasized that missed osteochondral injuries-present in up to 40% of cases—can lead to chronic pain and early patellofemoral arthritis [2,3]. Multiple anatomical abnormalities predispose to recurrence, including trochlear dysplasia, patella alta, increased tibial tubercle–trochlear groove (TT-TG) distance, and generalized laxity [5,6]. Dejour et al. demonstrated higher recurrence risk when TT-TG exceeds 20 mm or when patella alta is present [6]. Younger patients also have a higher likelihood of recurrence [5].
Although conservative management remains standard for first-time dislocations without large osteochondral fragments, several studies suggest that early MPFL reconstruction may benefit patients with high-risk anatomy. Smith et al. reported improved short-term stability with reconstruction compared to conservative care, though long-term outcomes remain debated [7]. In this case, the combination of MPFL rupture and osteochondral injury increased the recurrence risk. Persistent instability despite physiotherapy justified MPFL reconstruction, consistent with current evidence. Her successful return to sport aligns with outcomes reported in adolescents undergoing similar procedures.
Early identification of risk factors, structured rehabilitation, and timely surgical intervention when indicated are essential for preventing chronic patellofemoral instability and long-term cartilage degeneration.