Tracheo-Bronchial Compression by Massively Dilated Pulmonary Artery- a Rare Cause of Weaning Failure
Dr Ganesh KM*, Dr Padmakumar AV, Dr Pooja PS and Dr Chandan GS
Department of Medical Intensive care unit, Fortis Hospital Bannerghatta Road Bengaluru, Karnataka , India
*ORCID iD- 0009-0007-2374-2372
*Corresponding author
Ganesh KM, Department of Medical Intensive care unit, Fortis Hospital Bannerghatta Road Bengaluru, Karnataka , India
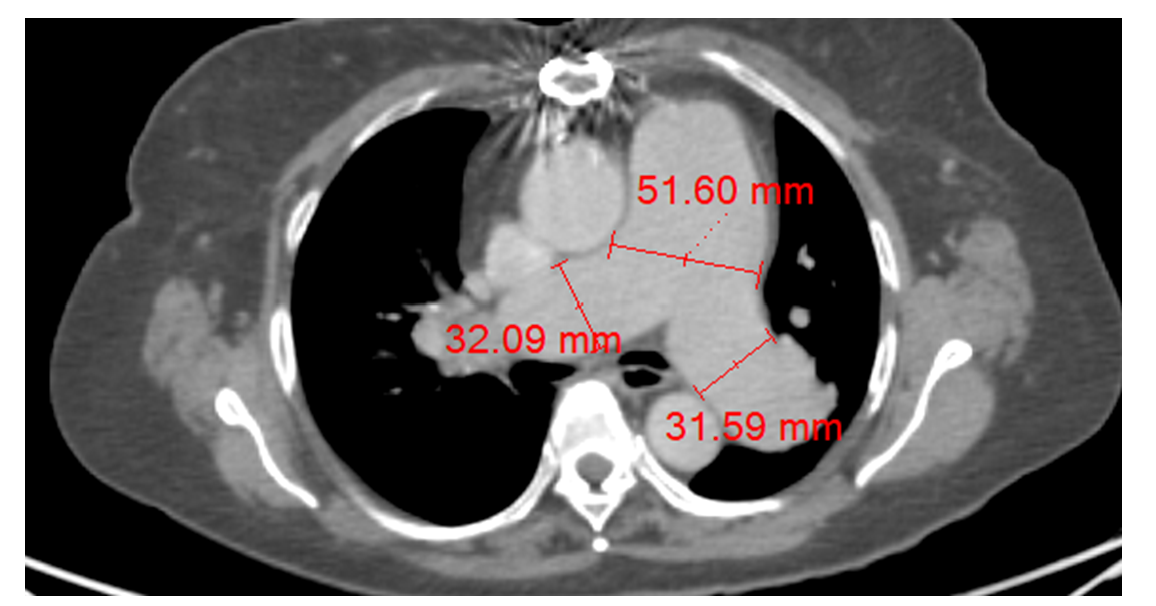
Figure 1a: Massively dilated Main Pulmonary artery(51.6mm),Left Pulmonary artery(31.59mm) and Right Pulmonary artery(32.09mm). Normal cutoff - main pulmonary artery 27mm, Left pulmonary artery
21mm and right pulmonary artery 19mm2
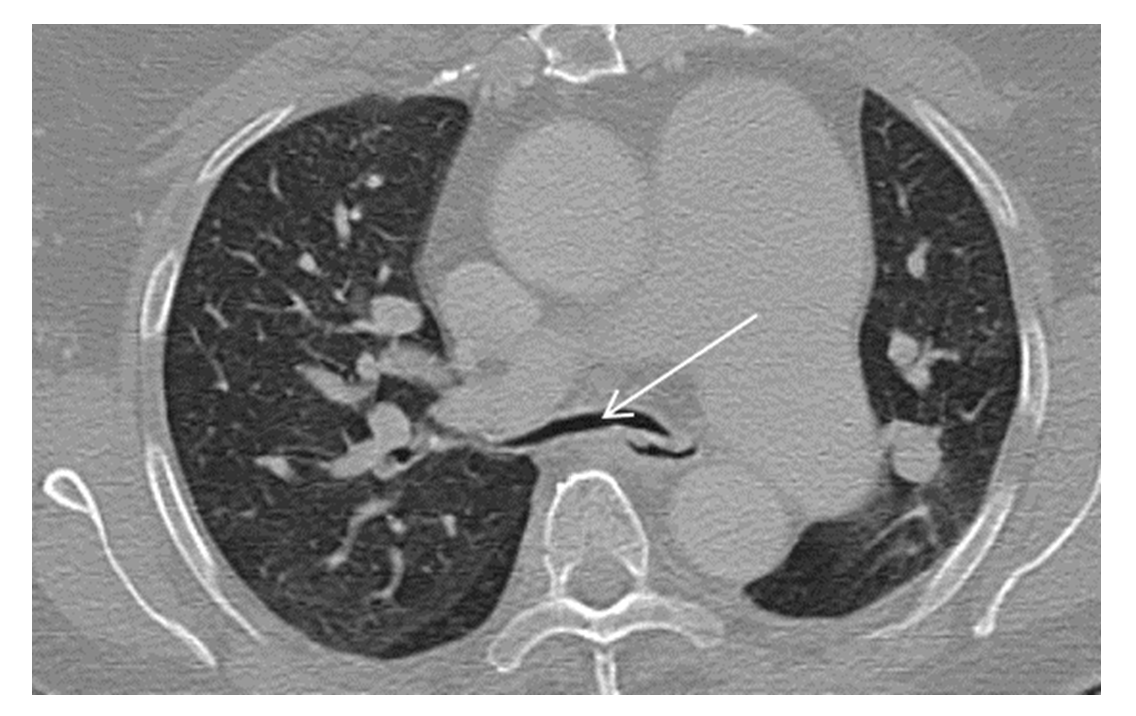
Figure 1b: Severe tracheomalacia(arrow), lung parenchyma showing emphysematous changes.
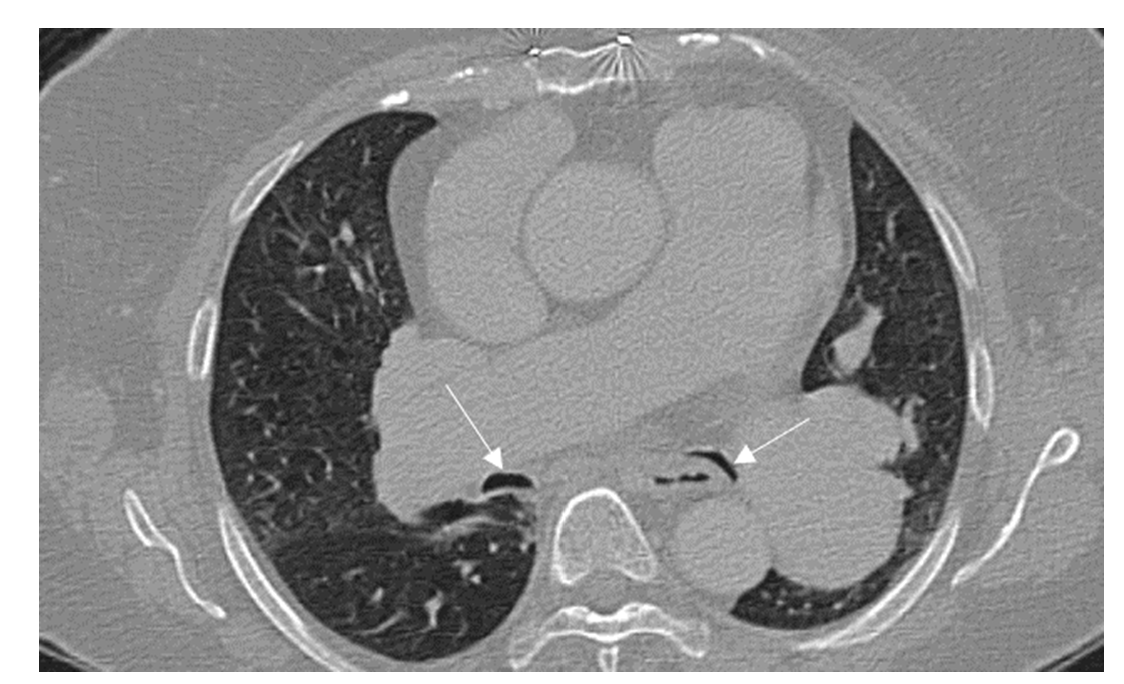
Figure 1c: Severe right and left bronchomalacia(arrows), lung parenchyma showing emphysematous changes.
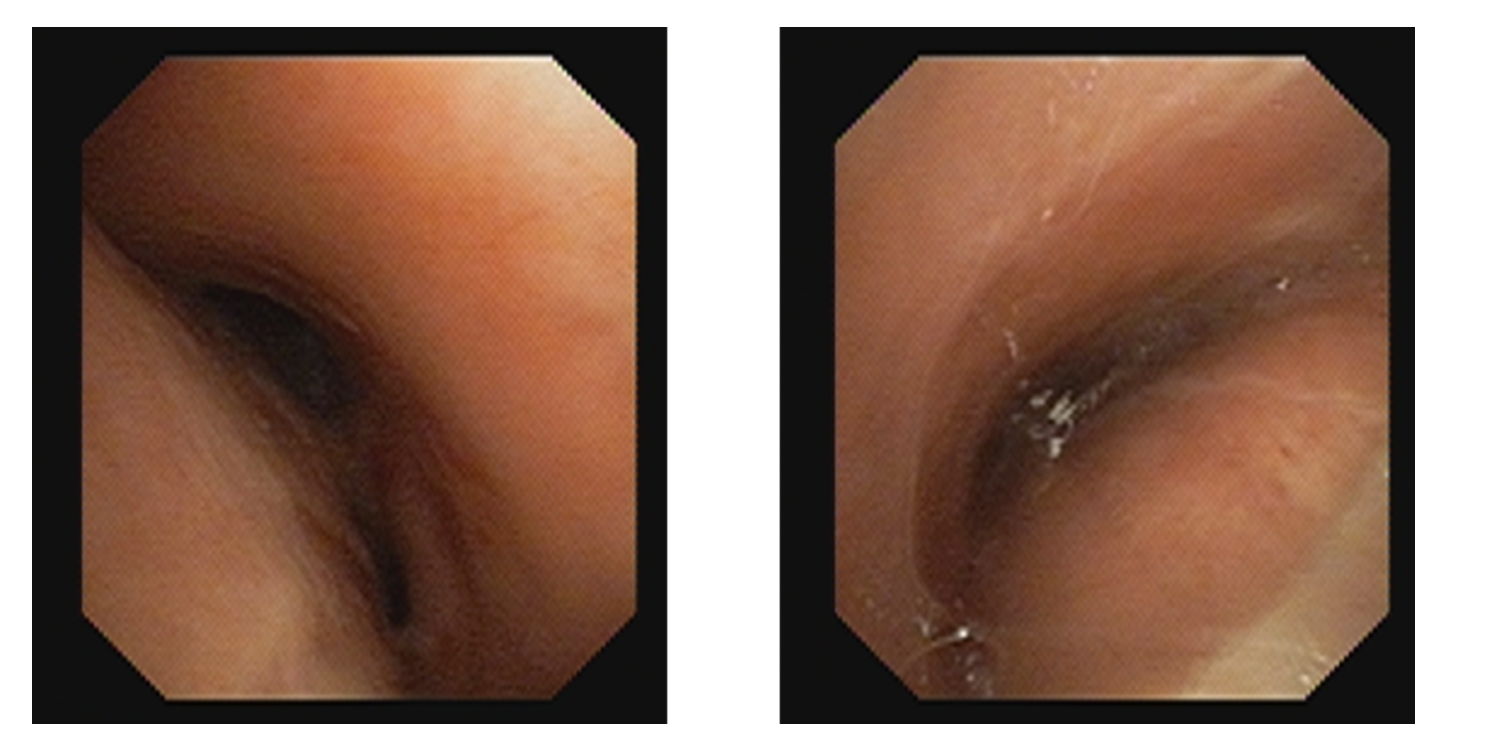
Figure 2: Bronchoscopy images showing severe trachea-bronchomalacia.
- Dakkak W, Tonelli AR (2016) Compression of adjacent anatomical structures by pulmonary artery dilation. Postgrad Med 128(5): 451-459.
- Pulmonary Hypertension and Pulmonary vascular disease, Webb,Muller and Naidich`s High Resolution CT of the Lung, Sixth edition, Wolters Kluwer, pp. 556-557.