This was a 50 year old woman with a history pertinent for recurrent, severe Major Depressive Disorder (MDD) and insomnia, as well as comorbidities of migraine with aura, hypertension, chronic kidney disease, and chronic low back pain. Surgical history was notable for cervical disc replacements secondary to degenerative disease, laparoscopic sleeve gastrectomy, and total abdominal hysterectomy for uterine fibroids. She presented for evaluation after a long history of episodically variable depressed mood, anhedonia, concentration deficits, and feelings of worthlessness; symptoms had been present for approximately ten years prior to presentation and arose within the context of military, familial, and occupational stressors. Numerous psychotropic trials of sufficient duration and dose were completed, including SSRIs, SNRIs, bupropion, buspirone, stimulants, non-benzodiazepine hypnotics, and first generation H1 antagonists. The patient additionally completed several courses of psychotherapy and a trial of transcranial magnetic stimulation (TMS). These therapies had varying efficacy, with many medications proving to have negligible effect or intolerable side effect profiles for the patient, or would prove efficacious until new stressors emerged, such as family dynamics or the COVID-19 pandemic and associated lockdown. TMS showed some improvements in overall mood, but this effect was transient and symptoms recurred over the subsequent months. Mood symptoms worsened, culminating in a suicide attempt using a combination of prescribed cyclobenzaprine and over-the-counter eye drops containing tetrahydrozoline hydrochloride. Given her treatment-resistant, persistent, and worsening depression, she was considered a candidate for ECT, and initial work-up was obtained, including CBC, CMP, EKG, head imaging, chest x-ray, and spinal x-ray imaging.
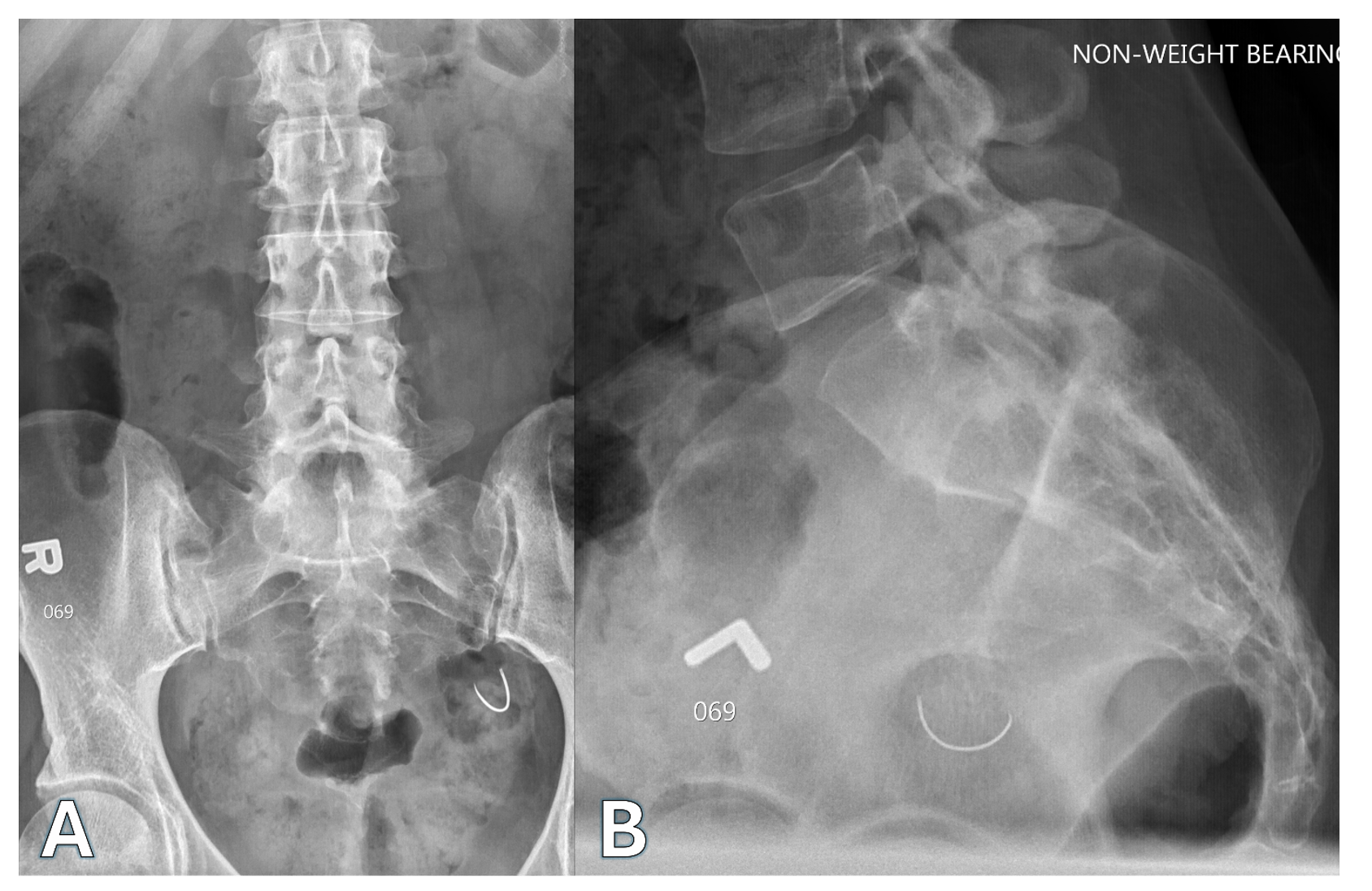
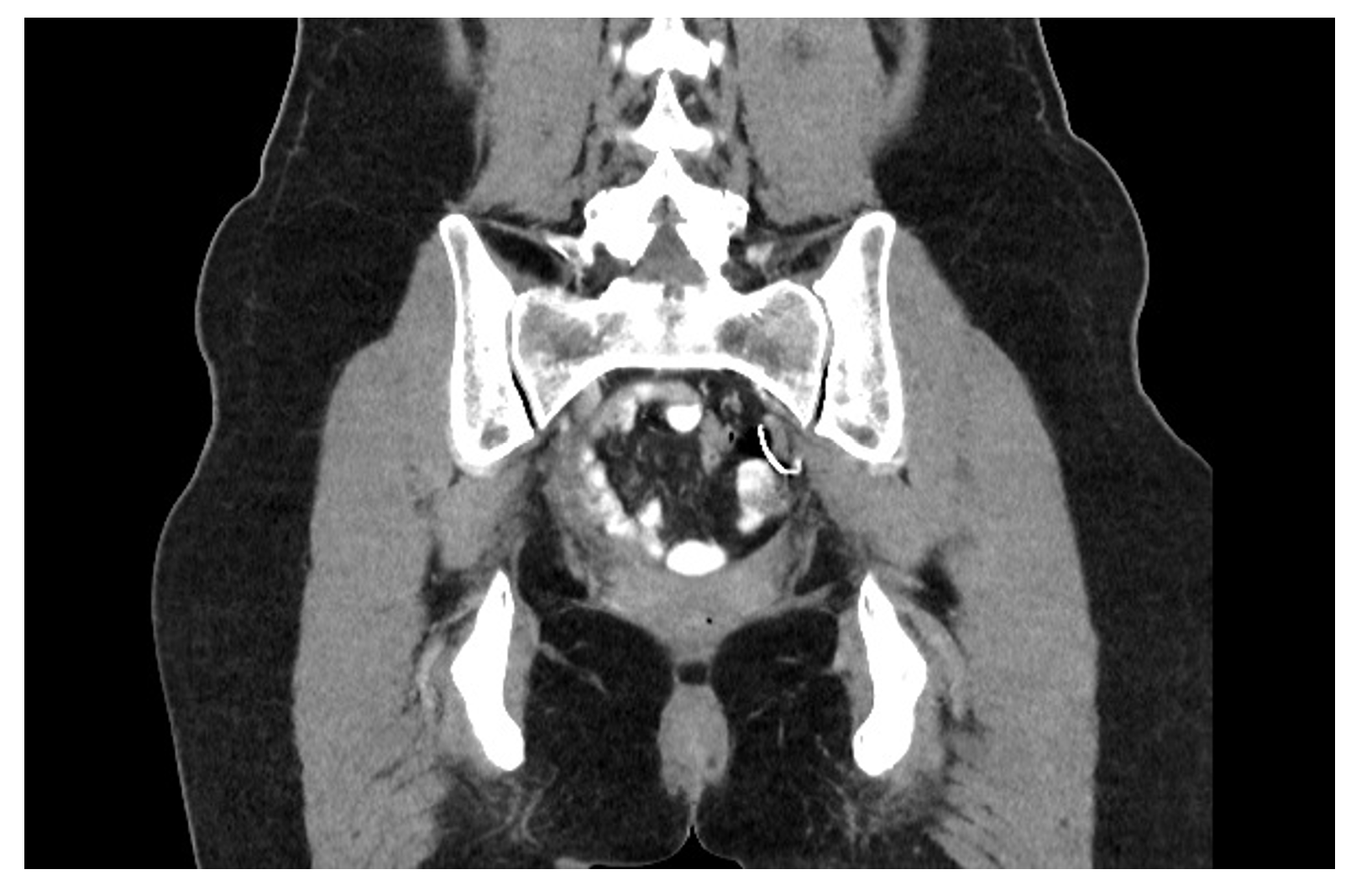
During initial work-up, three-view lumbar spine imaging (Figure 1) revealed mild degenerative changes and a “curvilinear, needlelike metallic foreign body in the left pelvis.” A follow-up CT abdomen-pelvis (Figure 2) confirmed this finding of a curvilinear metallic body in the left hemipelvis, most compatible with a retained surgical suture needle. She denied any abdominal pain or other GI symptoms. On directed questioning, the patient noted having been advised previously of “a wire” in her abdomen that had been seen previously on an incidental single-view anterior-posterior plain film four years prior. However, no additional workup or evaluation had been completed at that time, and she denied ever being advised that the object was likely retained from prior surgery.
During risk-benefit review of proceeding with ECT, concern was noted for the potential risks associated with increases in intra-abdominal pressures either displacing the needle or provoking spontaneous damage of nearby structures. General Surgery was consulted for this finding and confirmed with the patient the likelihood of this being a retained surgical needle from her hysterectomy six years prior. The possibility of future erosion into surrounding structures was also reviewed, however it was determined that the object’s placement and position posed no immediate contraindication to proceeding with ECT at that time. Following this discussion, the patient indicated that given the severity of her depression she would prefer to avoid postponing ECT. She discussed her concern that awaiting removal of the foreign body would delay her psychiatric care, and was advised that she could follow up with general surgery at any point in the future for object removal.
The patient was counseled on routine monitoring during treatments to include new abdominal or pelvic pain, presence of blood during toileting, or any additional new symptoms to suggest complication related to the object. In addition, routine review of complete blood counts was maintained to monitor for surreptitious bleeding. An ECT index series was initiated via right unilateral stimulation using the Thymatron System IV (Somatics, LLC) and a combination of propofol anesthetic with succinylcholine paralytic. Over the course of treatment, the patient was transitioned to bitemporal stimulation and the anesthetic was transitioned to methohexital. Overall improvements in symptomatology were noted with marked recovery of mood, energy, and diminished anxiety, and she was subsequently transitioned to maintenance treatments. At the time of publication she had received over 70 treatments with no gastrointestinal, abdominal, or pelvic symptoms suggesting complication.