Prevalence and Pattern of Smoking among Primary Health Care Patients
Almoutaz Alkhier Ahmed1*, Nazar Khalid Zarroug2, Mohamed Elfadel Abbas3, Samer Mohammed Syed4, Mohammed Abd Elmoneim Alyas5, Gais Mohamed Osman6,Khalid Mohydin7 and Aisha Abdulrahman Alzarooni8
1A/Professor -MBRU, SSR family medicine -Nad Alhamar Health Center. DAHC
2SR family Medicine – Nad Alhamar Health Center – DAHC
3SR family Medicine - Nad Alhamar Health Center – DAHC
4SR family medicine -Nad Alhamar Health Center – DAHC
5SR family medicine -Nad Alhamar Health Center – DAHC
6SR family medicine -Nad Alhamar Health Center – DAHC
7SR family medicine -Nad Alhamar Health Center – DAHC
8Consultant Family Medicine, Head of Nad Alhamar Health Center – DAHC
*Corresponding author
Almoutaz Alkhier Ahmed, A/Professor -MBRU, SSR family medicine -Nad Alhamar Health Center. DAHC
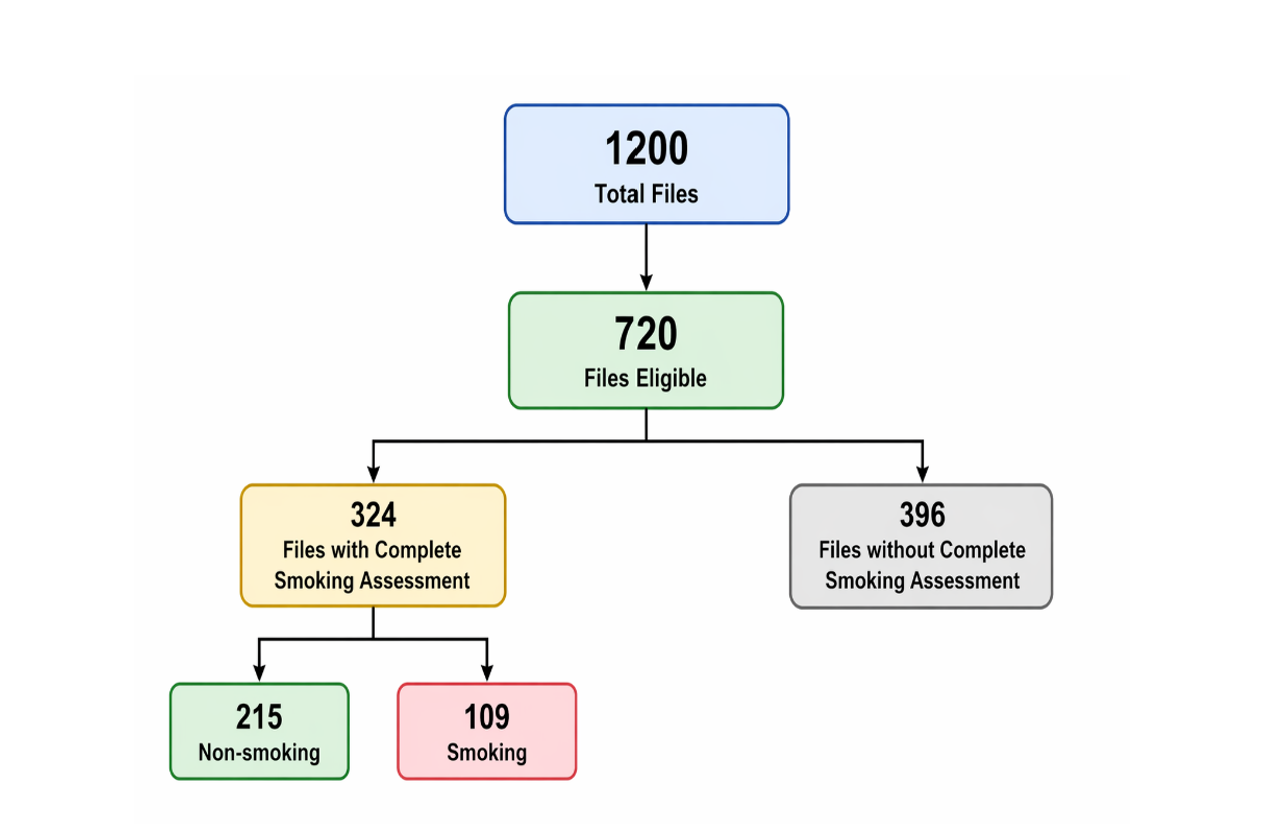
Figure 1: Sample selection.
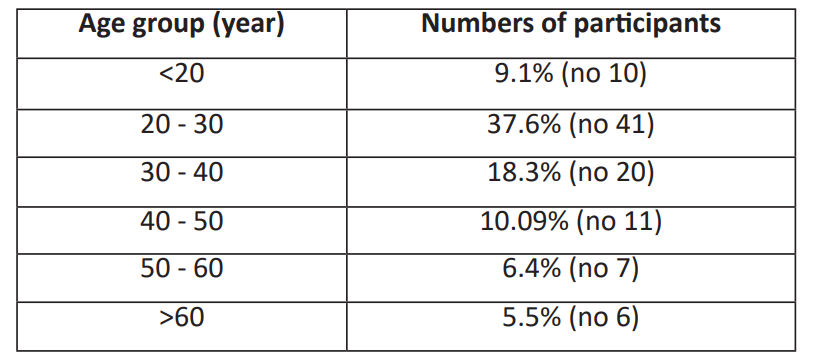
Table 1: Smoking by Age distribution.
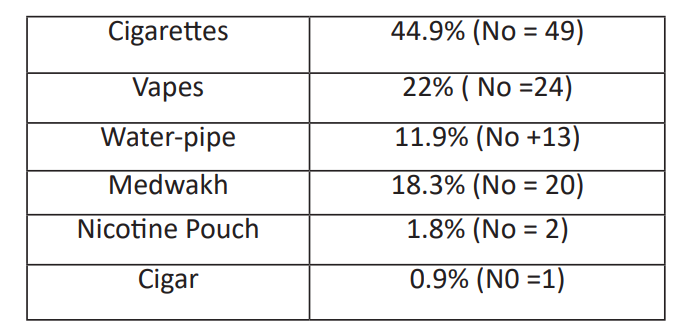
Table 2: Pattern of smoking.
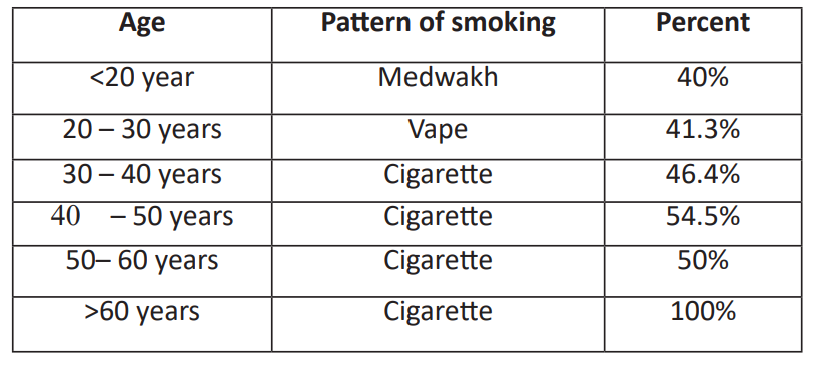
Table 3: Distribution of smoking pattern per age.
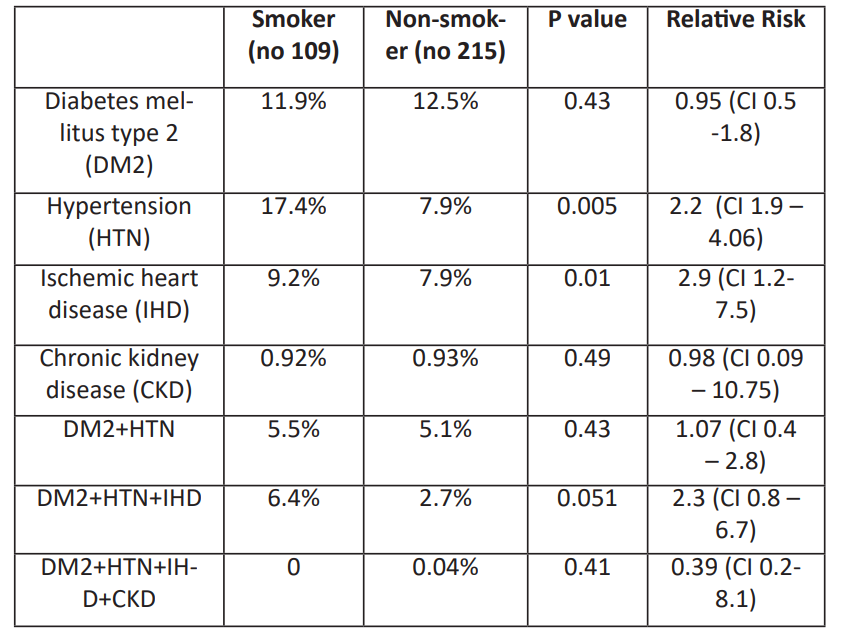
Table 4: Associated Non-communicable Chronic Diseases (Diabetes mellitus type 2, Hypertension, Ischaemic heart disease and chronic kidney diseases in smoker vs non-smokers.
- West R (2017) Tobacco smoking: Health impact, prevalence, correlates and interventions. Psychology & health 32(8): 1018-1036.
- Burki TK (2021) WHO releases latest report on the global tobacco epidemic. The Lancet Oncology. 22(9):1217.
- Alkhateeb BF, Altamimi AA, Ferwana MS (2020) Knowledge attitude and practices towards water pipe smoking among adults in saudi arabia: findings from a cross-sectional study. Journal of health informatics in developing countries. 14(1).
- Varghese J, Gharde PM (2023) A comprehensive review on the impacts of smoking on the health of an individual. Cureus 15(10).
- AlMulla A, Mamtani R, Cheema S, Maisonneuve P, Abdullah BaSuhai J, et al. (2021) Epidemiology of tobacco use in Qatar: prevalence and its associated factors. PLoS One. 16(4): e0250065.
- Dubai Health Authority (2025) Dubai Household Health Survey,2019. Dubai Household Health Survey_EN2022450248.pdf.accessed on 31/12/2025
- Obaid HA, Hassan MA, Mahdy NH, ElDisouky MI, Alzarba FE, et al. (2015) Tobacco use and associated factors among school students in Dubai, 2010: intervention study. East Mediterr Health J 20(12): 765-773.
- Crookes A, Wolff K (2014) Prevalence of the tobacco product dokha among high school students in Dubai. Subst Use Misuse 49(10):1349-1352.
- Aden B, Karrar S, Shafey O, Al Hosni F (2013) Cigarette, water-pipe, and medwakh smoking prevalence among applicants to Abu Dhabi’s Pre-Marital Screening Program, 2011. Int J Prev Med 4(11): 1290-1295.
- Al-Houqani M, Ali R, Hajat C (2012) Tobacco smoking using Midwakh is an emerging health problem–evidence from a large cross-sectional survey in the United Arab Emirates. PLoS One 7(6): e39189.
- Al Shemmari N, Shaikh RB, Sreedharan J (2015) Prevalence of dokha use among secondary school students in Ajman, United Arab Emirates. Asian Pac J Cancer Prev 16(2):427-430.
- Alraeesi FH, Farzin FJ, Abdouli KA, Sherif FY, Almarzooqi KA, et al. (2020) Smoking behavior, knowledge, attitude, and practice among patients attending primary healthcare clinics in Dubai, United Arab Emirates. Journal of Family Medicine and Primary Care. 9(1): 315-320.